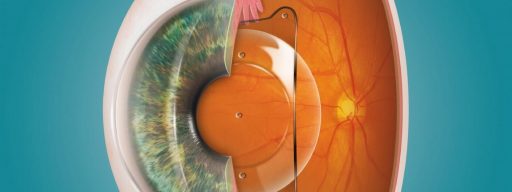
Laser refractive surgery is used to change the shape of the cornea, which is the eye’s main refractive optical medium. Cornea shape modification deviates and normalizes the path of the rays entering the eye.
Laser refractive surgery (LRS) allows the restoration of vision at far and near distances. Most often, it is used in patients with myopia (nearsightedness) of various degrees. This procedure is also indicated for hypermetropia (farsightedness), astigmatism, and presbyopia.
- PRK – photorefractive keratectomy.
- LASIK – laser in situ keratomileusis.
- SMILE – small-incision corneal lenticule (lens) extraction.
When performing PRK, the surgeon first removes the corneal epithelium and then ablates (or vaporizes) the corneal surface using an excimer laser.
During LASIK, the corneal flap (i.e. superficial corneal layer) with the hinge is cut using a microkeratome or femtosecond laser. The flap, having a thickness of 100–130 microns, is lifted and folded to the side, exposing the deeper layers of corneal stroma, which are then reshaped using an excimer laser ablation.
In the SMILE technique, a femtosecond laser only is used. The laser cuts the lenticule inside the central portion of the cornea. The surgeon then removes the lenticule with forceps or a spatula through a micro-incision of about 2 mm wide.

You can make an appointment by phone from 8:30 to 19:30 (daily).
For laser refractive procedures, two types of laser systems are used most commonly:
- Excimer laser (to vaporize or ablate the corneal tissue).
- Femtosecond laser (for precise cutting of the corneal tissue).
Laser refractive surgery helps solve vision problems and is an excellent alternative to other types of optical correction such as glasses or contact lenses. LRS is recommended to eliminate various refractive errors in:
- Myopia with or without astigmatism.
- Hyperopia with or without astigmatism.
- Astigmatism of various types.
Before surgical treatment, the patient consults with the ophthalmologist and undergoes thoughtful ophthalmic examination. Comprehensive examination helps to exclude some pathologies that would make laser vision correction undesirable.
In some cases, laser vision correction is contraindicated:
- Refractive disorder is not stable and is progressing.
- There is an ocular co-morbidity.
- There is increased intraocular pressure.
- The cornea is too thin.
Time in the operating room takes no more than half an hour, but a successful result requires careful preparation:
- Diagnostics and examination by a specialist.
- Computer calculation of the surgical plan.
During the preoperative phase, the ophthalmologist will choose the optimal surgical technique according to the individual parameters of the patient’s eye, deciding whether it is advisable to use the «knifeless» technique. In that case, only laser devices, no blades, will be used to cut the cornea.
The ophthalmologist also decides whether or not to use so-called «customized» or individualized ablation-in which the data of the corneal topographer and/or aberrometer are entered into the computer program for calculation of the exact parameters of the surgical procedure.
Surgery itself consists of the following steps:
- The patient is prepared for surgery.
- Local anesthesia and intravenous sedation are performed.
- Laser energy is applied to the cornea.
- The surgeon instills antibiotics and anti-inflammatory drugs.
- A temporary patch is applied.
Immediately after surgery, the patient may experience some sensation in the form of itching or burning. Visual acuity improves the first day after the procedure and continues to recover during the early postoperative period (up to 3–4 weeks).
Patients must follow the regime of instilling eye drops and refrain from physical activity for a while. Compliance with all the recommendations will help in regaining visual function as early as possible.
Currently, there is no single ideal method of surgical correction of refractive errors that suits all patients equally. The surgeon will select the best option by taking into account the individual anatomical characteristics of the patient’s eye, their visual needs, and lifestyle.